The Strasys Maternity Index (SMI) is a new way to track and understand maternity risk across NHS Trusts in England. Using 58 different measures from national maternity data, the Index helps identify where risks are highest, based not just on current performance, but also on how things are changing over time.
What the Index measures
The SMI looks at three key things:
- Current performance: how a Trust is doing now, based on clinical, safety, and outcome indicators relative to all England trusts providing maternity services.
- 12-month trend: whether things are improving, static or deteriorating.
- Birth volume: how many people are affected, based on the number of births at each Trust.
The final score combines all three, giving the clearest picture of maternity risk by quality, trend and scale.
100
Clinical, safety, and outcome measures from national maternity data
3
Dimensions scored: current performance, 12-month trend, birth volume
All
English NHS trusts providing maternity services are included in the Index
What the data shows
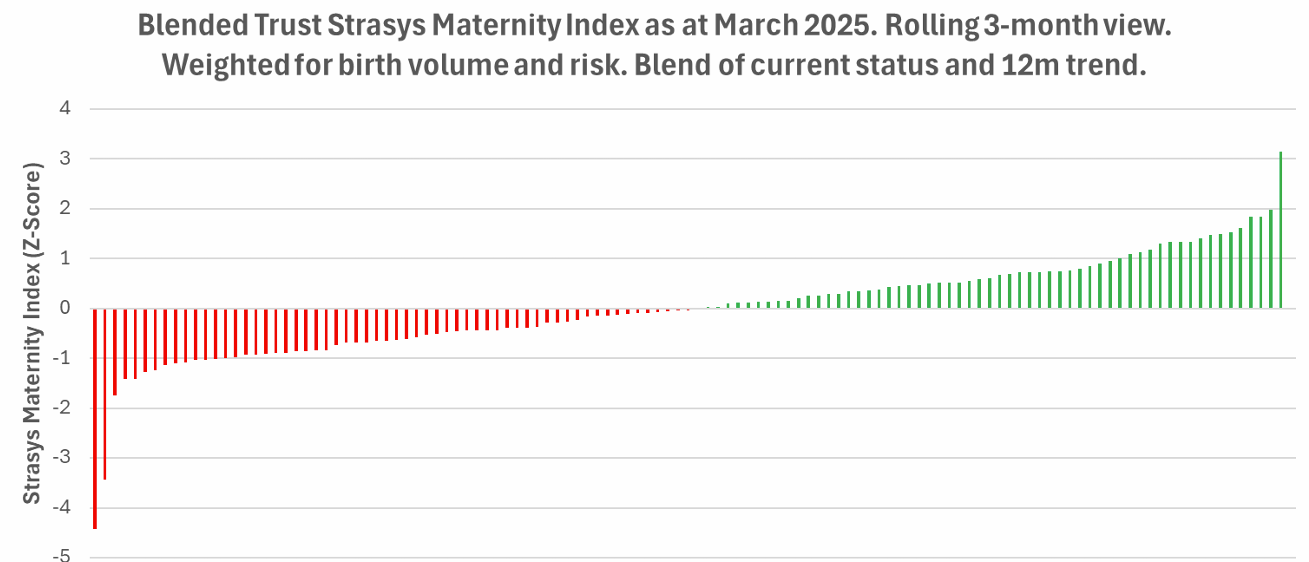
The Index highlights two large-volume trusts that stand out as being of particular concern. One Trust in particular combined a high number of births, a top-five risk score, and a clear 12-month decline in key clinical areas such as neonatal health (Apgar scores), post-partum haemorrhages, and perineal trauma.
At the other end of the spectrum, Homerton Healthcare appears to have a substantial lead over other trusts in the low risk it poses to the system relative to the high volume of births managed by that trust.
How the score is calculated
Each Trust’s score is built using:
- Z-Score comparison to normalise individual metrics across England.
- A weighting system that gives greater importance to risk factors and measures of higher clinical concern.
- Measures averaged over rolling periods to reduce impact of outlier months, and measures disregarded where low volumes could distort findings.
- A trend analysis using 12 months of data to see if things are getting better or worse.
Why volume matters
Some Trusts have high risk scores but serve very few patients. To focus on system-wide risk, the Index adjusts for birth volume, showing which Trusts present the greatest risk to overall patient safety based on how many people they serve.
Why this matters
The SMI gives leaders a clear, data-driven view of where maternity risks lie, how they’re changing, and how many people are likely to be affected. It’s designed to support smarter decision-making, helping the NHS focus on where action is most needed.
Maternity claims remain the single largest category of NHS clinical negligence litigation. The cost of getting this wrong is measured in lives and in billions. The SMI provides the intelligence to act before an incident, not after one.

Mark Jennings
Chief Solutions and Services Officer, Strasys
Common questions
The SMI measures three dimensions of maternity risk: current clinical performance relative to all English trusts providing maternity services, the 12-month trend showing whether performance is improving or deteriorating, and birth volume showing how many people are affected. These combine into a single composite score.
The SMI uses 58 different measures drawn from national maternity data, including clinical indicators such as Apgar scores, post-partum haemorrhage rates, and perineal trauma, along with safety and outcome metrics.
Some trusts have high risk scores but serve very few patients. Adjusting for birth volume focuses attention on system-wide risk, showing which trusts present the greatest risk to overall patient safety based on how many people they serve.
Each trust’s score is built using Z-Score comparison to normalise metrics across England, a weighting system giving greater importance to higher clinical concern risk factors, measures averaged over rolling periods to reduce outlier impact, and trend analysis using 12 months of data.